A tooth abscess is a dental illness that is characterized by a pus-filled pocket that develops in or around a tooth and causes pain and discomfort. This condition can cause swelling, pain, fever, and an unpleasant taste after eating. The most frequent causes of this bacterial infection include dental decay left untreated, gum disease, and tooth damage. Good oral hygiene practices, routine dental exams, and obtaining emergency dental treatment if any symptoms appear are examples of some preventative measures you can take. In this article, we will discuss what is tooth abscess, its causes, treatments, side effects, and preventative measures.
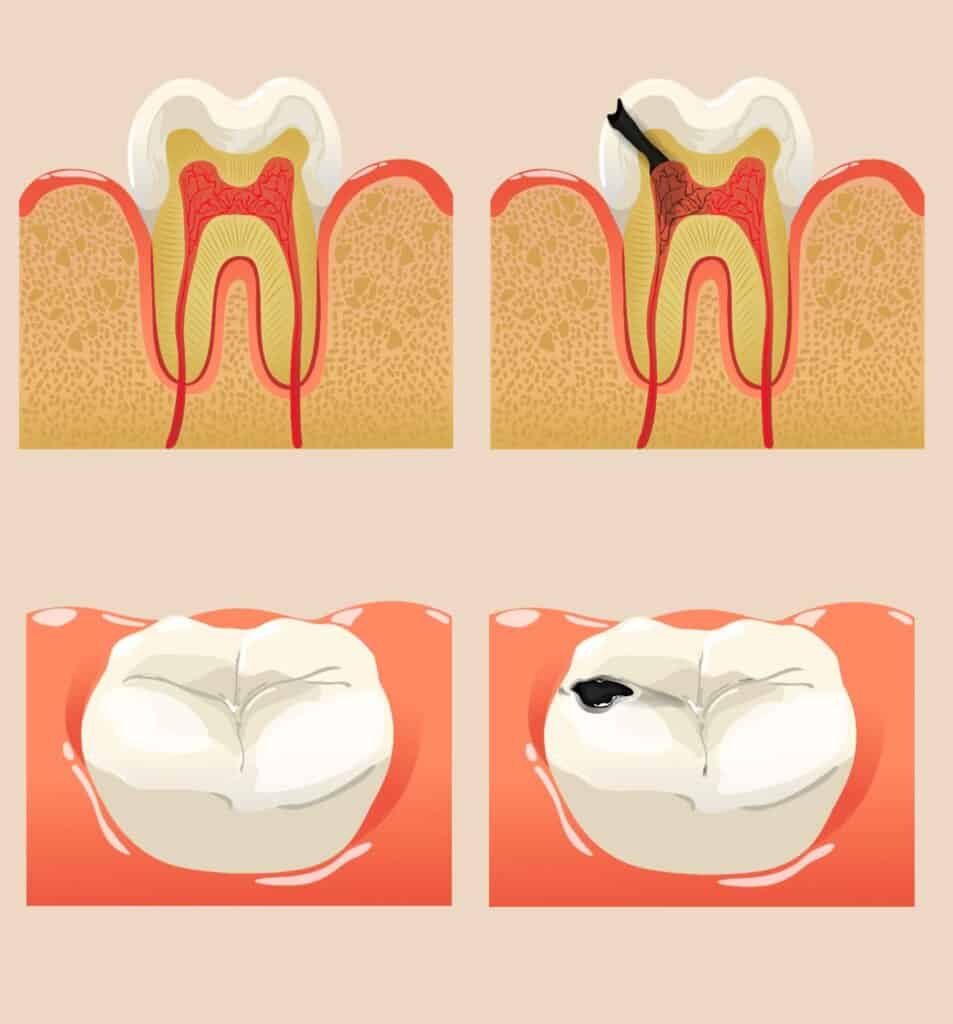
What is a tooth abscess?
As we said before, tooth abscess is a bacterial infection that causes a pus pocket beneath the root of the tooth. This can come as a result of different dental issues such as; untreated cavities, failed dental work, or an injury, and develops next to the tooth root in the gums. An abscessed tooth will cause discomfort and pain in your mouth, ears and neck area.
If you start to notice any symptoms of this bacterial infection, you should visit your dentist right away since it is considered a dental emergency. The infection should be drained by either a root canal procedure or a tooth extraction. While you wait for your dental appointment, there are several remedies available that may help reduce the pain and discomfort.
Types of Dental Abscesses
There are 3 different types of dental abscess:
- Periodontal abscess
- Periapical abscess
- Combined periodontal-endodontic abscess
Symptoms
The first and most common indicator of a tooth abscess is the presence of pain and discomfort in the area of the affected tooth. This pain has been described as a persistent, throbbing sensation that seems to emerge suddenly and intensify as time passes. A tooth abscess can remain asymptomatic for a long time, even for years, before causing a toothache. The throbbing pain experienced in both the teeth and gums may extend to affect adjacent areas such as the neck, ear, or jaw, becoming increasingly unbearable. This discomfort can affect normal activities like chewing or eating.
The swelling in the upper or lower jaw may become apparent when the illness worsens and causes the lymph nodes in the area to grow. Additionally, people may experience frequent headaches, nausea, fever, poor breath, and an unpleasant aftertaste when they eat. They may also become sensitive to hot and cold meals and beverages.
Causes & Risk Factors
Tooth abscesses are mostly caused by untreated cavities, tooth decay, injury to the tooth, or failed dental work. You are more prone to develop cavities if you:
- Consume a diet high in sugar and carbohydrates
- Poor dental hygiene
- Mouth breath
- Smoke or drug use
- Use antibacterial dental hygiene products that disrupt the oral microbiome
- Lack of vitamin K2 and D3
- Damage to the teeth or jaw
If you neglect your dental health, cavities can form, and an untreated cavity can damage the pulp, which is the center of the tooth, where the blood vessels and nerves are located. When the bacteria enters this area it causes inflammation, swelling, and pus. When this occurs the damage can be reversed but when it is caused by failed dental work, the damage is done and you cannot retrieve the tooth.
When the pressure starts to build up, you will start to feel a sharp pain in your jaw. At this point, the abscess has been formed and it should be drained by a professional, before causing further damage. After draining, the pain will go away, but it doesn’t mean that the infection will. Furthermore, it should be addressed in the additional visits that the dentist will set for you.
Treatments
Depending on the severity of the illness, your dentist will first prescribe pain killer medicine to reduce the infection and after that, he will need to perform a root canal or tooth extraction to address the tooth abscess and relieve the pain. Later on, a dental implant procedure will be needed to address this issue.
The tooth abscess will not go away on its own once it has developed. It may rupture on its own, which will relieve the pain and make you think the problem has gone away but this is not true. Furthermore, let’s take a look at the potential treatments your dentist may use to treat tooth abscesses.
Antibiotics
Tooth abscess pain is typically addressed through antibiotic treatment, which serves to alleviate swelling and inflammation. Antibiotics are now less often used because of the rise in antibiotic resistance brought on by their misuse in previous years. As a result, doctors can decide to postpone providing antibiotics until they can determine the infection’s diagnosis. It is important to understand that antibiotics will not treat the tooth abscesses, but rather they provide pain relief and they operate as a band-aid until a more effective procedure, such as an extraction or root canal, can be carried out.
Pain Relief Medication
As we previously stated, painkillers and antibiotics are only prescribed to provide temporary relief before a root canal or tooth extraction procedure. The most effective painkillers for dental pain are non-steroidal anti-inflammatory medications and paracetamol, which are also used to treat tooth abscesses. The most frequently prescribed medications by dentists to relieve pain and discomfort are:
- Ibuprofen (Advil)
- Naproxen (Aleve)
- Celecoxib (Celebrex)
- Aspirin (Motrin)
Root canal procedure
The most common method of treating an infection that has developed into a tooth abscess is a root canal. Tooth abscess will develop only when the pulp of your tooth is dead and unable to be retrieved. Most dentists will try to save the remaining tooth structure with a root canal before treating your tooth abscess. When treating a dental abscess, endodontic treatment is typically chosen as the first option.
When a dentist considers performing a root canal procedure on a patient, they carefully assess several key success indicators. These indicators help ensure the procedure is both secure and likely to be effective. Some of the factors they take into account include:
- Manageable tooth Canals: The dentist evaluates whether the canals within the tooth can be effectively worked on. Complicated or unusually shaped canals can increase the risk of re-infection and may influence the decision to proceed with a root canal.
- Calcification: The absence of calcified canals is a positive indicator, as calcification can make it challenging to access and treat the infected area within the tooth.
- Likelihood of Success: Dentists assess the overall likelihood of a successful procedure, taking into consideration factors like the extent of infection and the condition of the tooth’s structure.
- Advanced Imaging: Cone-beam CT (CBCT) scans are often used to provide a highly accurate and detailed image of the tooth’s root anatomy. This advanced imaging helps the dentist plan and execute the root canal procedure with precision.
It’s important to note that following a root canal, it is common practice to protect the tooth from potential breakage by placing a dental crown. The crown helps reinforce the tooth’s structure and prevent any damage that could occur due to the tooth becoming more brittle after the removal of its pulp. This final step in the root canal process ensures the long-term stability and functionality of the treated tooth. Patients should discuss their specific case with their dentist to understand the necessity of a dental crown and the overall success of the root canal procedure.
Benefits:
A dental crown is essential for maintaining a tooth’s foundational strength and ensuring that chewing and orthodontic growth are unaffected. A feasible alternative to more extreme procedures like tooth extraction is this non-invasive method. Having a tooth extracted is considered more expensive and invasive than having a root canal procedure performed. Another advantage of having a root canal performed is the prevention of bone loss. In conclusion, choosing a dental crown and implant may be the best option for preserving oral health.

Risks:
Undergoing a root canal procedure, while often effective in treating dental issues, does come with certain considerations. One possible risk, which should be taken into consideration is not proper cleaning, which can leave bacteria behind. This can lead to further development of the infection.
You should also consider the risk of tooth fracture after a root canal since the tooth structure may become more fragile. Additionally, the development of a new infection may have chronic effects and it can result in a systemic infection.
Furthermore, the success of a root canal procedure is highly dependent on its proper execution. Errors such as underfilling or overfilling the affected area can fail, necessitating additional procedures like a second root canal or even tooth extraction. Therefore, it is crucial to weigh these factors and consult with a dentist to make informed decisions regarding root canal treatments while considering all potential risks and outcomes.